
Heart Attack: Myocardial Infarction (MI) - Your Guide to Recovery. Welcome to California Pacific Medical Center. Note: Please review this information about your health condition. We want you to be involved in the decisions affecting your care. If you have family members, caregivers, or friends caring for you, please have them read this information. Each person has a unique health condition. 
If you have any questions, please ask the doctors, nurses, and therapists caring for you. A heart attack occurs when there is a blockage of blood flow in one or more of the coronary blood vessels (arteries) that supply blood to your heart muscle (See Figure 1). Figure 1. Back to top. How Does a Heart Attack Occur? Many heart attacks are caused by . An unstable plaque is a fatty deposit that triggers an inflammatory response in the body. This inflammatory process causes plaque deposits to weaken and rupture. When plaque ruptures, a blood clot can form partially or completely blocking the artery. The area of the heart muscle supplied by the artery no longer receives enough blood and oxygen. Figure 2. After a heart attack, scar tissue forms in the damaged muscle. The remaining heart muscle works harder to pump blood through the body. When your heart muscle is damaged, electrical irregularities in the rate or rhythm of the heart may develop. Chest x- ray: A chest x- ray can show abnormal heart size and signs of heart failure (poor pumping by the heart). You may also receive the following tests to further evaluate your condition: Echocardiogram: A non- invasive test to evaluate the structure and motion of heart function, heart valves, and blood flow through the heart. Echocardiogram uses ultrasound (high- frequency sound waves) to create an image of your heart on a television screen (monitor). This test identifies whether an area of your heart has been damaged by a heart attack. Infarction .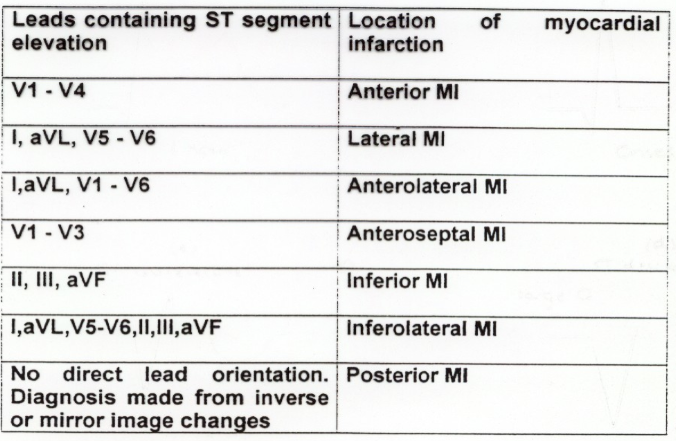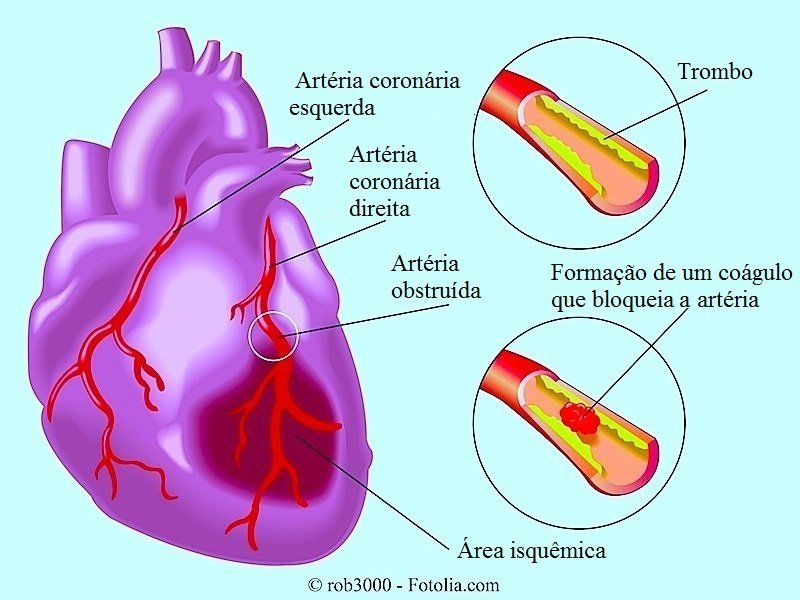  
Cardiac Catheterization & Coronary Angiogram: Cardiac catheterization is an invasive, non- surgical procedure. A coronary angiogram is a specialized x- ray procedure that is done as part of a cardiac catheterization. A cardiac catheterization and a coronary angiogram are done to study the structure of the arteries that bring blood to the heart muscle and to evaluate the function of the main pumping chamber of the heart. During a cardiac catheterization, the cardiologist inserts a small hollow tube (catheter) into an artery or vein and then advances it into the heart. 
Acute myocardial infarction: A heart attack. The term "myocardial infarction" focuses on the heart muscle, which is called the myocardium,and the changes that occur. The cardiologist injects contrast (x- ray dye) through the catheter to outline the arteries to show any blockages or narrowings that may exist within them. Myocardial Perfusion Imaging (MPI) “Stress Testing” (Persantine Thallium): These tests help identify blood flow problems to your heart. Small amounts of a radioactive material are injected into your bloodstream through your IV. Special cameras can detect the radioactive material as it flows through your heart. Back to top. Understanding Your Medications. Your doctor will order medications to: Reduce blood clotting. Control your pain. Stabilize your heart rhythm, if necessary. Lower your blood pressure. Prevent further damage to your heart. Your medications may include: Blood- thinning medications (anticoagulants and antiplatelets): Blood- thinning medications prevent blood clots from forming in the blood. Aspirin, Coumadin (Warfarin), Heparin, Integrilin (Eptifibatide), Lovenox (Enoxaparin), Plavix (Clopidogrel), and Reo. Pro (Abciximab) are used to make the blood less sticky and less likely to clot. When taking these medications report any unusual bleeding to your doctor. Nitrates: These medications, used to treat chest pain, open narrowed blood vessels and improve blood flow to the heart. A Segment Elevation Myocardial Infarction (STEMI) occurs when a coronary artery is totally occluded by a blood clot. Learn the symptoms and treatment. Unstable Angina and Non–ST-Segment Elevation Myocardial Infarction: --Part II. Coronary Revascularization, Hospital Discharge, and Post-Hospital Care. Examples include: Imdur (Isosorbide Mononitrate), Isordil (Isosorbide Dinitrate), Nitro- Bid (Nitroglycerin oral) Nitroglycerin IV, and Transderm- Nitro (Nitroglycerin topical). Pain Relievers: Morphine is often given intravenously to relieve chest pain. Thrombolytics: These medications, often called clot- busters, dissolve a blood clot that is blocking the blood flow in a coronary artery. Beta- Blockers: These medications reduce the workload of your heart. A beta- blocker is usually started at a low dose and gradually increased over time. Common beta- blockers are Coreg (Carvedilol), Inderal (Propranolol), Lopressor or Toprol- XL (Metoprolol), and Tenormin (Atenolol). ACE Inhibitors: These medications help your heart pump effectively by relaxing the blood vessels. Some common ACE Inhibitors are Altace (Ramipril), Capoten (Captopril), Lotensin (Benazepril), and Zestril or Prinivil (Lisinopril). Calcium Channel Blockers: These medications relax the muscle of the blood vessels and may slow your heart rate. Common calcium channel blockers are Calan or Isoptin (Verapamil), Cardene (Nicardipine), Cardizem (Diltiazem), and Norvasc (Amlodipine). Cholesterol- lowering drugs: A variety of medications such as statins, niacins, and fibrates can help lower your cholesterol. Examples of statins include: Lipitor (Atorvastatin), Zocor (Simvastatin), Mevacor (Lovastatin),and Pravachol (Pravastatin). Optimal management of myocardial infarction in the subacute period focuses on improving the discharge planning process, implementing therapies early to prevent. Myocardial infarction, commonly known as a heart attack, is the irreversible necrosis of heart muscle secondary to prolonged ischemia. This usually results from an. Examples of niacins: Nicotinex (OTC), Slo- Niacin (OTC) (Nictonic Acid,Vitamin B3). An example of a fibrate: Lopid (Gemfibrozil). Note: Make sure to tell your doctor about any non- prescription drugs you may be taking, such as cold remedies, sleep aids, or herbal medications. Back to top. Percutaneous Coronary Intervention (PCI) and Other Procedures. PCI is a treatment procedure that enlarges narrowed coronary arteries without performing surgery. Your cardiologist will determine the most appropriate treatment for your condition during this procedure. Treatment will vary from patient to patient. PCI may include one or more of the following treatment strategies: Balloon catheter angioplasty: A small balloon is placed in the narrowed area of the artery and inflated with liquid. This pushes the plaque (blockage) to the sides of the artery where it remains. This technique restores the opening of the artery. The cardiologist removes the balloon at the end of the procedure. Stent: The cardiologist places a small, hollow metal (mesh) tube called a “stent” in the artery to keep it open following a balloon angioplasty (See Figure 3). This technique prevents constriction or closing of the artery during and after the procedure. Figure 3. Rotational Atherectomy: Calcium build- up is removed from the blood vessel using a specialized instrument. You may experience some discomfort such as chest pain, pressure or tightness in your chest during the procedure. Please let the staff know if you are feeling any discomfort during the procedure. Medications may be given to ease the discomfort. Brachytherapy: This technique delivers radiation treatment to prevent scar tissue from growing back in the area of a previously implanted stent. If this treatment is recommended, a doctor who specializes in radiation therapy will speak with you and will answer any questions you may have about brachytherapy. Coronary Bypass Surgery: In rare cases, emergency coronary bypass surgery may be performed at the time of a heart attack. Bypass surgery involves sewing veins or arteries in place at a site beyond a blocked or narrowed coronary artery. Back to top. Planning Your Activity. Your doctor may suggest a cardiac rehabilitation program for you. Cardiac rehabilitation services are designed to help you to recover faster and to return to a full and productive life. Phase I Cardiac Rehab – Begins in the hospital with physical therapy, occupational therapy, and a nutritional consult. Phase II Cardiac Rehab – An outpatient program comprised of an exercise program, education, and counseling. Phase III Cardiac Rehab – A continuation of the above and support for heart- healthy lifestyle changes. For more information on cardiac rehabilitation classes at California Pacific, call (4. Back to top. Live a Heart- Healthy Lifestyle. Obtain Regular Medical Checkups. Conditions such as high cholesterol, high blood pressure, and diabetes, may be present without any symptoms in the early stages. Smoking increases your heart rate and blood pressure, contributes to atherosclerosis (build- up of plaque in your blood vessels), and decreases oxygen to your heart. Cigarette smoking is a major risk factor for another heart attack. Smoking is an addiction. Nicotine releases a chemical to your brain which gives you a feeling of pleasure. Your doctors and nurses realize that smoking is not an easy habit to quit, and we want to support you. Here are some tips: Make the decision to quit smoking while you are in the hospital. Inform your doctor and nurse. Ask your doctor to prescribe a treatment plan to help you stop smoking. Your doctor may order medications to help with nicotine withdrawal and smoking cessation. These include nicotine replacement therapy (patch or gum), a smoking avoidance medication, or an antidepressant medication. Ask your doctor if these medications are appropriate for you during your hospitalization and after you go home. Inform your doctor or nurse when you are experiencing symptoms of nicotine withdrawal such as anxiety, cravings, irritability, restlessness, depression, and insomnia. Call 1- 8. 00- NO- BUTTS for more information about smoking cessation. Exercise Regularly. Exercise helps improve heart muscle function following a heart attack. It also helps you maintain a healthy weight and control risk factors such as diabetes, high cholesterol, and high blood pressure. You are encouraged to exercise regularly. Regular exercise can reduce your symptoms. Follow These Guidelines: Rest after meals. Wait at least 1 hour after you eat to walk or do any strenuous activities. Space your activities to avoid getting too tired. Exercise (walk or cycle) at a calm, easy pace. Pace yourself so you can easily hold a conversation while you exercise. Exercise when you are rested. NOTE: If you become short of breath, dizzy, develop pain or chest tightness – stop and rest. If symptoms persist - Call 9. Maintain a Healthy Weight. NSTEMI: Non- ST- Segment Myocardial Infarction Explained. Non- ST segment elevation myocardial infarction (NSTEMI) and ST- segment elevation myocardial infarction (STEMI) are both commonly known as heart attack. NSTEMI is the least common on the two, accounting for around 3. NSTEMI, STEMI, and a third condition called unstable angina are all forms of acute coronary syndrome (ACS). For its part, ACS is defined as any condition brought on by a sudden reduction or blockage of blood flow to the heart. Understanding Acute Coronary Syndrome. All forms of ACS are usually caused by the rupture of plaque in a coronary artery, leading to either partial or complete obstruction of the vessel. Depending on the severity of the obstruction, ACS can be classified into three different types: Unstable angina is the partial rupture of an artery which causes chest pains. Unlike stable angina (which occurs when you exert yourself), unstable angina can occur anytime and is considered more serious. Despite the symptoms, unstable angina does not cause permanent damage to the heart. STEMI is considered a . We can differentiate STEMI from NSTEMI by readings on an electrocardiogram (ECG) in the so- called . During a heart attack, the ST- segment is raised. As such, NSTEMI gets its name because there is no evidence of ST segment elevation. Because NSTEMI causes damage to the heart muscle, doctors will still consider it a heart attack (some might say a . With that being said, NSTEMI has more in common with unstable angina and, as such, usually has better outcomes. Emergency Treatment of NSTEMITreatment of NSTEMI is identical to that of unstable angina. If a person appears with cardiac symptoms (chest tightness, clamminess of the skin, shooting pains in the left arm, etc.), the doctor will begin intensive therapy to stabilize the heart and prevent further damage. Stabilization would primarily focus on two things: Eliminating acute ischemia, a condition in which the heart is not getting enough oxygen, causing cell death. This is done, in part, by administering beta blockers to prevent damage caused by the excessive production of adrenaline and high- dose statins to stabilize ruptured plaque and reduce arterial inflammation. The use of these drugs will usually alleviate cardiac ischemia within minutes. Oxygen and morphine will typically be given to assist respiration and reduce pain. Stopping blood clot formation involves the use of aspirin, Plavix, and other medications to thin the blood and prevent the clumping of platelets. It also includes the avoidance of . Many cardiologists will use a TIMI (thrombosis in myocardial infarction) score to determine the likely outcome for the individual. The TIMI score assesses whether if the person has any of the following risk factors: Age 6. Presence of at least three risk factors for coronary heart disease. Prior coronary blockage of greater than 5. ST- segment deviation on the admission ECGAt least two angina episodes in past 2. Elevated cardiac enzymes. Use of aspirin within the past seven days. If the person has two or fewer of these risk factors (TIMI score 0- 2), the need for further intervention can often be avoided. If the score is higher, the cardiologist may want to perform a cardiac catheterization with angioplasty and stenting. For persons who decline invasive treatment, a stress test will typically be performed prior to discharge. If there are any signs of continued cardiac ischemia, invasive therapy will be strongly advised. Sources: Amsterdam, E.; Wenger, N.; Brindis, R.; et al.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. Archives
November 2017
Categories |
 RSS Feed
RSS Feed
